Oral Health: A Key Determinant In Health (2024)
[lwptoc hierarchical=”1″]
Scientific research in the medical field shows this constantly: health starts from the mouth.
This article summarises some research on why oral health is so important, not just to our teeth and gums but to our overall health. In particular, it explores the science of our oral microbiome.
What Is The Oral Microbiome?
The oral cavity is inhabited by a variety of microorganisms – this is what we call our oral microbiome.
The oral cavity harbours the second most complex microbiome in the body, after the gut.
This quote immediately helps us understand the significance of the oral microbiome. Many of us now know that our gut microbiome has a critical role to play in modulating our immune system (and thus inflammatory state), nervous system, detoxification, and metabolic health among others. So we can start to appreciate that perhaps our oral microbiome has similar characteristics.
The below image summarises what conditions/organs/glands have been associated with imbalances in the oral microbiome.
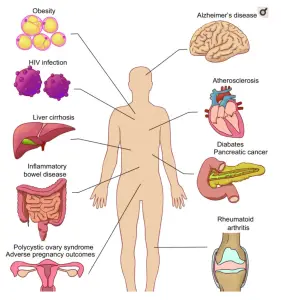
How Oral Health Effects Overall Health
Oral health has potentially multi-organ systemic implications.
How can bacteria residing in our moth has such an impact on systemic health?
The mouth constitutes an entry point to the respiratory and digestive systems, and it is highly vascularised. With leaky gums bacteria or/and components of bacteria are able to ‘leak’ into the circulatory and lymphatic systems where they can then travel around the body. The result is low level chronic systemic inflammation.
It is generally believed that this low-grade inflammation will negatively impact the health of the whole body or/and worsen other systemic diseases already present.
Researchers now believe that, in the general population, chronic periodontitis may be an important source of “invisible peripheral inflammation”. Thus, periodontitis is also called “low-grade systemic disease”, affecting a variety of systemic diseases.
What proportion of the population has periodontitis? There are estimates in the research of 40-50%!
What Are The Symptoms Of Periodontitis?
- Bad breath or bad taste that won’t go away
- Red or swollen gums
- Tender or bleeding gums
- Painful chewing
- Loose teeth
- Sensitive teeth
- Gums that have pulled away from your teeth
- Any change in the way your teeth fit together when you bite
- Any change in the fit of partial dentures
Risk Factors For Periodontitis
- Smoking
- Diabetes
- Poor oral hygiene
- Stress
- Heredity
- Crooked teeth
- Underlying immune-deficiencies.
- Fillings that have become defective
- Taking medications that cause dry mouth
- Bridges that no longer fit properly
- Female hormonal changes, such as with pregnancy or the use of oral contraceptives
Oral Health And Gut Health
There are two routes by which the oral microbiome might influence gut health:
- Through the simple act of swallowing bacteria. The oral bacteria “invade the intestines”, causing imbalances in the gut microbiome and affecting organs of the digestive system. (source)
- Via the bloodstream. Oral bacteria, especially periodontitis pathogens, can enter the bloodstream through damaged tissue (i.e. gums) where they then enter systemic circulation. Once here they can travel around the body and might end up in the gut (but can end up in the knee driving rheumatoid arthritis, or in the brain driving dementia.
Let’s look at two conditions in particular.
Oral Health And Colorectal Cancer
Fusobacterium nucleatum is a common oral bacterium that is enriched in colorectal adenomas and adenocarcinomas. In humans, high fusobacterial colorectal cancer abundance is associated with chemo-resistance and poor prognosis. In animal models, fusobacteria accelerate colorectal cancer progression.
Targeting Fusobacterium nucleatum may reduce fusobacteria cancer progression and therefore determining the origin of colorectal cancer Fusobacterium nucleatum and the route by which it reaches colon tumours is of biologic and therapeutic importance.
Research has suggested that colorectal cancer Fusobacterium nucleatum may originate from the oral cavity.
Fusobacteria in the mouth may travel to colorectal cancer via the aforementioned routes: the digestive tract, or, via blood caused by chewing, daily hygiene activities, or dental procedures.
Oral Health And SIBO
There is also research discussing the role of the oral microbiome as a potential cause of SIBO. This is super important to consider for anyone suffering with chronic SIBO that doesn’t respond long term to typical interventions.
Oral Health And Alzheimer’s Disease
There is evidence that bacteria found within the oral cavity can promote amyloid-beta formation and contribute to Alzheimer’s pathology (source). The accumulation of amyloid-beta plaques in the brain is a central pathological feature of Alzheimer’s disease. It is believed that amyloid responses may be a result of the host immune response to pathogens in both the central nervous system and peripheral systems.
It’s pretty clear there is a significant correlation between oral health and Alzheimer’s. Let’s look at the evidence.
In one study, 152 people were followed for 20 years. The results found that the severity of periodontitis and the cognition level had an inverse relationship in subjects with fewer than 10 teeth missing. (source) The more teeth were missing the greater the risk of cognitive decline.
Another longitudinal aging cohort study of 144 people showed that those with the APOE-ε4 gene, and fewer teeth, have a faster cognitive decline than people without these two risk factors. (source)
One study conducted a 32-year survey of 597 participants (all male). The results showed that tooth loss, the depth of periodontal pockets, and the degree of alveolar bone loss were related to cognitive impairment, particularly in those older than 45. (source)
A survey of 5468 subjects found that irregular tooth brushing was associated with Alzheimer’s disease. (source)
A survey of 2355 people (60 years and older) found that there is an association between periodontitis and cognitive impairment (source)
What bacteria have been associated with Alzheimer’s?
- Porphyromonas gingivalis.
- A. actinomycetemcomitans.
- Treponema denticola.
- Fusobacterium nucleatum.
- Actinomycin meyeri
It’s important to appreciate further research is needed on these organisms and their relationship with Alzheimer’s.
Concluding Thoughts
Numerous factors contribute to the onset of Alzheimer’s disease, ranging from lifestyle choices to genetic predispositions and environmental influences. Of particular note are chronic oral inflammatory conditions like periodontitis, which holds significance due to its close proximity to the brain. Periodontitis, a persistent inflammatory condition linked to the microbiome, affects individuals across all age groups and tends to persist as they age. Research suggests that certain oral bacteria, including P. gingivalis, T. forsythia, and T. denticola, may exacerbate inflammatory processes in the central nervous system (CNS) associated with Alzheimer’s disease.
Moreover, other oral pathogens could also contribute to local and CNS inflammation, potentially influencing the development of Alzheimer’s. Through routine activities such as oral hygiene practices and eating, these oral pathogens introduce their byproducts into the brain via pathways known as the oral-brain axis. Over time, these microbial byproducts and inflammatory agents may continuously stimulate immune cells within the CNS, such as microglia, leading to a cascade of events including neuroinflammation, increased amyloid beta production, and neuronal cell death—hallmark characteristics of Alzheimer’s disease. These immune dysfunctions within the central nervous system can then show up as cognitive impairments, including memory deficits.
Oral Microbiome & Cancer
Among the systemic conditions influenced by the microbiome, cancer has not been an exception. We have learned that chronic infections contribute to carcinogenesis, with approximately 13% of the global cancer burden being directly attributable to infectious agents (source)
There were reports of a correlation between periodontitis and leukeamia as early as the late 1940s early 1950s. Since those pioneer studies, there is mounting evidence of the correlation between periodontal disease and various cancers. Several meta-analyses have confirmed the suspicion that periodontal disease should be considered as a risk factor in several types of cancers. In fact in a meta-analysis by Corbella et al., they found that a statistically significant association was found for all cancers studied, both combined and individually (digestive tract, pancreatic, prostate, breast, corpus uteri, lung, hematological, eosophageal/oropharyngeal and Non-Hodgkin lymphoma). (source)
Oral Microorganisms and Cancers Outside the Oral Cavity
One characteristic of the oral microbiome that distinguishes from other body sites is that many oral microorganisms that are considered commensals in the oral cavity are commonly associated with various cancers in distant organs. (source)
The associations of oral organisms and distant cancers occur in two categories. The first appears in certain types of cancer where no oral microbes are directly involved in the tumour’s pathogenesis, but there is a consistent change in the composition of the oral microbiome associated with cancer, thus with the potential use of those changes as biomarkers of cancer. The second kind of association is the association of organisms involved in tumourigenesis, such as F. nucleatum association with colorectal cancer. (source)
There are three types of associations between microbiome and disease that have been described as potential biomarkers in cancer:
- Increase or decrease in numbers of individual organisms.
- Use of models of several organisms as predictors and assessing their performance.
- Changes in diversity indexes that give an overall picture of the behaviour of the community.
As examples of specific organisms as biomarkers, an increase in F. nucleatum has been linked to colocrectal cancer, and P. gingivalis and Fusobacterium spp. have been linked to pancreatic cancer.
Oral Microbiome, Mastication, & Cognition
We also need to be mindful of how mastication and poor oral health can influence the ageing process, both directly and indirectly. Miquel et al (2018) discussed the current evidence and suggested that a deterioration in mastication and oral health during ageing can have:
- Direct effects on systemic health through mechanisms such as the migration of the oral microbiota into the systemic environment (i.e oral bacteria into the bloodstream)
- Indirect effects on systemic health through changes in nutrient intake.
They went on to say that a loss of teeth and reduction in masticatory efficiency during ageing can have:
- Direct effects on cognitive performance and potentially impact cognitive health through mechanisms such as enhanced adult hippocampal neurogenesis
- Indirect effects on cognitive health through changes in nutrient intake.
Miquel et al concluded that “oral health and masticatory efficiency are modifiable factors which influence the risk of poor cognitive and systemic health during ageing, although it is currently premature to propose chewing-based interventions to slow the rate of cognitive decline and improve cognitive health during ageing” (2).
Systemic Health Affects Oral Health Too
There is also clear evidence that certain systemic conditions influence our oral health too.
Systemic diseases such as diabetes, rheumatoid arthritis (RA), and systemic lupus erythematosus (SLE) increase susceptibility to destructive periodontal diseases.
Also in human studies and animal models, these diseases have been shown to enhance inflammation in the periodontium and increase the risk or severity of periodontitis.
Another layer of evidence is that successful RA treatment with anti-inflammatory drugs partially reverses oral microbial dysbiosis.
Oral Microbiome Testing
For my UK readers, Invivo Diagnostics offer an oral microbiome test.
For my US readers, Oral DNA, offer an oral microbiome test.
How To Improve Your Oral Health
Diet
- Focus on traditional oral hygiene practices – brush twice a day, and floss daily.
- Eat a diet rich in phytonutrients: plenty of fresh and ideally in-season fruit and vegetables.
- Avoid snacking/grazing throughout the day.
- Ensure good levels of fat-soluble vitamins, A, D, E, and K.
- The best source of vitamin A is liver.
- The best source of vitamin D is the sun.
- Vitamin E is found in fats and oils from animal products (meat, poultry, fish and dairy foods), as well as numerous plant foods including avocados.
- The best source of vitamin K2 is nato. I believe most of us need to be supplementing vitamin K2. Vitamin K can be found in dark green leafy vegetables.
- If you have periodontitis or receding gums, consider eating 2-3 meals per day, with no snacking.
- Ensure you’re not mouth breathing.
Stop Mouth Breathing
Mouth breathing induces a series of diseases.
Reductions in saliva flow result in extended periods of low pH, which disrupts a healthy oral–nasal–pharyngeal microbiome. Such conditions inhibit the growth of beneficial species and drive the growth of bacteria with an acid-producing/acid-tolerating phenotype, thereby increasing the risk of caries (dysbiosis). (source)
In one study comparing mouth to nasal breathers, the overall bacterial profiles differed between the two groups, and the differences were related to the duration of mouth breathing. The diversity of oral–pharyngeal microbiota was significantly higher, and the nasal–pharyngeal species tended to be consistent in the mouth-breathing group. Also, opportunistic pathogens were higher in relative abundance.
Interestingly, the expression level of oxidative-stress-related salivary proteins was up-regulated, while immune-related proteins were down-regulated in mouth breathing group.
Use A Tongue Scraper
Tongue scraping is also important for oral health; it is known that a significant cause of volatile sulfur compounds (VSCs), a major component of bad breath, is due to the bacteria coating the tongue. (source)
In one study both tongue scraping and tongue brushing were equally effective in reducing the plaque load in children. (source)
Best Toothpaste For Oral Health
For my UK readers, I recommend Gutology mineral toothpaste, or/and, RiseWell Toothpaste.
For my US readers, I recommend Boka.
Hydroxyapatite (HA) is a naturally occurring mineral form of calcium apatite, which is found in our bones and teeth. Using toothpaste containing hydroxyapatite can offer several benefits for oral health:
- Remineralisation: Hydroxyapatite can remineralise tooth enamel. It can help to repair early stages of tooth decay by depositing minerals back into the enamel, making it stronger and more resistant to acid attacks.
- Desensitising: Tooth sensitivity can occur due to exposed dentin or enamel erosion. Hydroxyapatite toothpaste can help reduce sensitivity by forming a protective layer over the exposed areas, shielding the nerves from external stimuli.
- Whitening: Hydroxyapatite toothpaste can also have whitening effects. It can remove surface stains from teeth, resulting in a brighter and more radiant smile over time.
- Gentle Cleaning: Unlike some abrasive ingredients found in traditional toothpaste formulas, hydroxyapatite particles are gentle on the enamel while still effectively removing plaque and bacteria from the teeth and gums.
- Reduction of Plaque Formation: Hydroxyapatite has been shown to inhibit the adhesion of bacteria to the tooth surface, thereby reducing plaque formation and potentially lowering the risk of cavities and gum disease.
- Bioactivity: Hydroxyapatite has a high degree of biocompatibility with tooth enamel, making it a safe and natural choice for oral care products. It integrates well with the tooth structure and supports overall oral health.
- Minimal Side Effects: Hydroxyapatite toothpaste typically has fewer side effects compared to some other ingredients commonly found in toothpaste, making it suitable for individuals with sensitive teeth or allergies to certain chemicals.
Best Mouthwash For Oral Health
I also like the RiseWell mouthwash.
Best Probiotic For Oral Health
Invivo Bio.Me Oral.
Best Tongue Scraper
For my US readers click here.
For my UK readers click here.
Recommended Book
- The Dental Diet by Dr. Lin: click here.
Summary
As Pete Williams discussed on the Healthpath podcast we are more microbe than we are human. And thus to understand ourselves, to understand how we can support someone back to optimal health we need to understand their microbes. More now than ever, it seems that the oral microbiome is just as important as the gut microbiome. One paper summed it up well:
Studies in oral microbiomes and their interactions with microbiomes in variable body sites and variable health conditions are critical in the cognition of our body and how to make an effect on human health improvement (4).
References
- Oral Dysbiosis in Pancreatic Cancer and Liver Cirrhosis: A Review of the Literature: click here.
- A practical guide to the oral microbiome and its relation to health and disease.: click here.
- The oral microbiome and human health: click here.
- In Sickness and in Health-What Does the Oral Microbiome Mean to Us? An Ecological Perspective: click here.